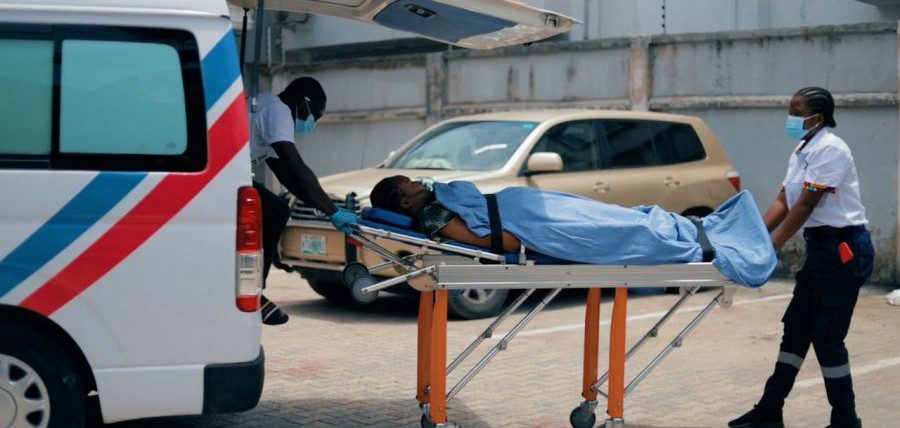
An industry report by Salvus Emergency has identified a lack of real-time data and digitalisation as a major factor preventing Nigeria’s emergency care system from functioning effectively.
The report titled “Nigeria’s Emergency Healthcare: The Coordination Crisis and the Unlocking of a Multi-Billion Naira Ecosystem” explained that Nigeria’s emergency response is a paradox of availability versus functionality. The gap is not about the lack of hardware, but rather in the coordination of available resources to meet demand.
With over 6 million medical emergencies estimated annually, the National Emergency Medical Services and Ambulance System’s (NEMSAS) coverage is less than 0.2%, revealing how the system deviates from reality amid a lack of informed data.

The system lacks data, revealing how actors operate blindly by sending ambulances to locations that no longer need them. While there is an ambulance (at least in cities), the coverage is low, as an average Nigerian relies on commercial buses or the kindness of strangers during emergencies.
Additional data further highlights these gaps.
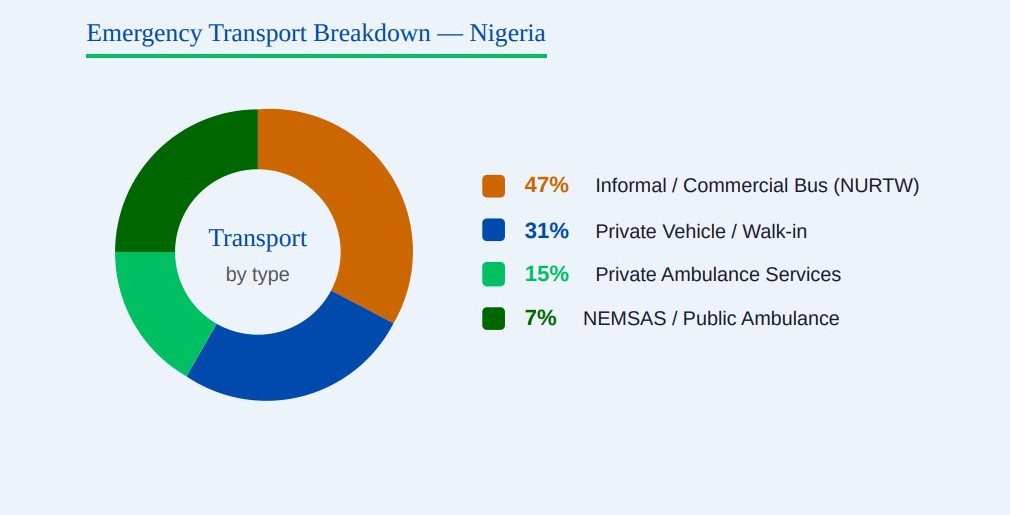
NEMSAS and Public Ambulances account for only 7% of total emergency transport. This means that for every 100 emergency cases, only 7 are transported using government-provided ambulances.
Private ambulance services account for 15% of emergency transport, while private vehicles and personal walk-ins account for 31%. Informal or commercial buses (NURTW) take the largest share of 47%, showing how public-use vehicles have been a rescue during emergencies.

In the same light, a lack of real-time data to detect emergencies or locations susceptible to emergencies impacts the time-to-care system.
While the World Health Organisation’s (WHO) standard for average response time during emergencies is 8 minutes, Lagos average is 17 minutes, rising to as much as 60 minutes in worst cases—still among the best response times in Nigeria.
The scenario is even worse for rural areas, which either wait for hours or get ignored owing to the coverage gap. States like Zamfara, Yobe, and Ebonyi are virtually ambulance deserts.
The dire impact of these gaps is terrifying.
An estimated 10-15% of Nigeria’s 1.6 million annual deaths occur within emergency departments; largely because patients arrived too late or without pre-hospital stabilisation.
Digital interventions
Given increasing digital adoption in Nigeria, the report encouraged a live dashboard for hospitals and NEMSAS showing available ambulance locations in real-time, with estimated time of arrivals (ETAs).
Also, digitalisation helps hospitals and medical personnel be aware of areas prone to emergency situations. This is made possible through the interpretation of data collected over time.
The report also suggests an integration with Google Maps or Waze for emergency vehicle routing and direct notification to traffic authorities. With this, ambulance software connects directly to Google Maps to find the fastest path to the emergency location. It also alerts road authorities (Police, FRSC) that an emergency vehicle is en route.


Hospitals are not left out. As standalone emergency responders (ERs) are failing, hospitals are encouraged to partner with coordinated dispatch platforms to reduce walk-in trauma deaths and improve bed management efficiency.
Although Nigeria’s emergency system is not yet at the global standard in terms of facilities, it can rescue lives by integrating digital systems for real-time data tracking and availability.
Also Read: SNG Health launches $30m local mosquito net manufacturing facility, Nigeria’s first.
Funding gaps impact data availability
Nigeria’s health care system is in a funding crisis, characterised by persistently low budgetary allocations, often below 5% of the total budget. This, in turn, contributes to data and technology gaps in the system.
Acknowledging this, Chief Executive Officer at Salvus Emergency, Emmanuel Oziuwa-John, noted that efforts to strengthen the system have been hindered by a lack of funds.
“There have been more attempts to clean up and strengthen the health sector, especially after COVID. We see this especially through specific data banks like DHIS2; funding is still terribly low for a nation like Nigeria,” he told Technext.
He concluded that, “so we can say there’s been some (funding) neglect.”


Emmanuel noted that health-based tech startups, organisations, and NGOs are doing the best they can in terms of rescuing the system and funding. Some have also built technology that connects to hospitals to provide medical logistics.
Ultimately, improving Nigeria’s emergency response system will depend on coordinated public-private efforts to build a unified, data-driven infrastructure.